Anti- VEGF injections alone can be considered for patients who are highly motivated and have no barriers to follow-up.PRP is usually preferred as treatment occurs in a single session (reduces risk of loss to follow-up).Both PRP and anti-VEGF therapy are equally effective.Proliferative retinopathy: PRP and/or anti-VEGF therapy.Severe NPDR: Treat as proliferative retinopathy with panretinal laser photocoagulation ( PRP) and/or anti-VEGF therapy.Mild NPDR to moderate NPDR: Observation only repeat dilated comprehensive eye examination every 6–12 months.For patients with significant vision impairment, consider:Įarly detection and treatment of diabetic retinopathy can prevent 90% of blindness.Arrange follow-up eye exams at regular intervals.Screen for additional microvascular complications of diabetes because of the high risk of co-occurrence.Continue aspirin if indicated for another condition.Initiate treatment for lipid disorders as indicated (see “ Guidelines for lipid-lowering therapy”).Treat hypertension if present (see “ Approach to management of hypertension”).Lifestyle recommendations for patients with diabetes mellitus.Antihyperglycemic treatment of diabetes.Refer all patients with diabetic retinopathy to an ophthalmologist.Noncenter-involving DME: ≥ 1 mm diameter retinal thickening that does not involve a central subfield.Center-involving DME: ≥ 1 mm diameter retinal thickening in a central subfield.If OCT has been performed, can be further categorized into:. 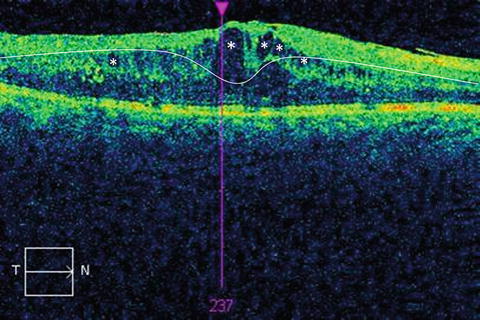
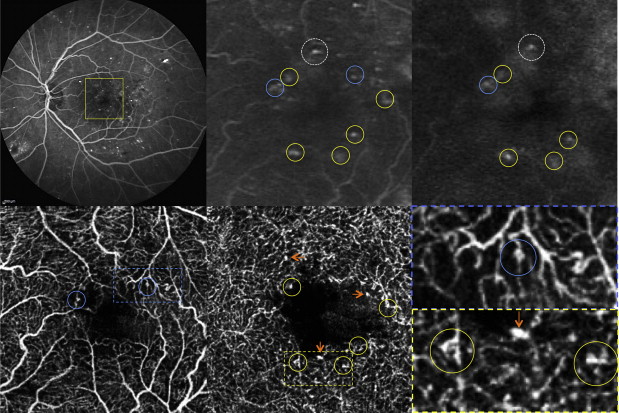
Within 1 disc diameter of the center of the macula: any zone of retinal thickening ≥ 1 disc size in any area.Hard exudates (if associated with adjacent retinal thickening).Within 500 microns of the center of the macula.Or elsewhere in the eye, if accompanied by vitreous and/or preretinal hemorrhage.On the optic disc or within 1 disc diameter.In ≥ 1 retinal quadrant: moderate intraretinal microvascular abnormalities.In ≥ 2 retinal quadrants: signs of ischemia (e.g., venous beading).In all 4 retinal quadrants: capillary microaneurysms, dot intraretinal hemorrhages.Mild intraretinal microvascular abnormalities or signs of ischemia.Capillary microaneurysms (to a greater extent than in mild NPDR).Vitrectomy may be required for patients with complications, e.g., tractional retinal detachment, vitreous hemorrhage PRP, focal and/or grid laser, and anti-VEGF therapy may be considered depending on severity.PRP (usually first-line) and/or anti-VEGF therapy.Severe: Consider PRP or anti-VEGF therapy.Mild-to-moderate: observation only reassess every 6–12 months.Treatment of diabetes and underlying ASCVD risk factors.May result from vitreous hemorrhage, retinal detachment, or neovascular glaucoma.May occur in all stages of NPDR and PDR.Clinically significant retinal thickening and edema involving the macula, associated hard exudates.Fibrovascular proliferation → vitreous hemorrhage, traction retinal detachment.Neovascularization is the hallmark of PDR.Findings of nonproliferative retinopathy are usually present.Intraretinal microvascular abnormalities (IRMA).Retinal vessel microangiopathy → blood leaks → retinal hemorrhages → retinal infiltration with lipids and fluid → macular edemaĮxamination findings ( dilated comprehensive eye exam or retinal photography).Retinal vessel microangiopathy → chronic retinal hypoxia → abnormal proliferation of blood vessels → traction on retina → retinal detachment.Retinal vessel microangiopathy → blood leaks → retinal hemorrhages.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
